Among the various causes of back discomfort, a herniated disc stands out as a common source of sharp, radiating pain. This condition affects the spine’s ability to function smoothly and can limit mobility. While the experience varies from person to person, understanding the underlying mechanisms of this spinal issue is the first step toward finding relief and managing the condition.
What Is a Herniated Disc?
The human spine consists of individual bones called vertebrae, which stack on top of one another to form the spinal column. Between each vertebra lies a rubbery cushion known as an intervertebral disc. These discs act as shock absorbers, allowing the spine to flex, twist, and bear weight without damaging the bones. A herniated disc occurs when the soft center pushes through a tear in the disc’s tougher exterior. This displacement can irritate nearby nerves. Age-related wear and tear is a primary cause. Other contributing factors include repetitive motions that stress the spine or traumatic injuries.
What Are the Symptoms?
Symptoms of a herniated disc vary greatly depending on the location of the injury and whether the disc is pressing on a nerve. Some people may have a herniated disc without knowing it, as it does not always cause noticeable issues. If the herniation occurs in the lower back, pain typically radiates from the buttocks down the leg and into the foot. This specific type of pain follows the path of the sciatic nerve. If the issue lies in the neck, the discomfort usually manifests in the shoulder and arm.
Beyond pain, individuals might experience specific sensations related to nerve compression. Numbness or tingling can occur in the body part served by the affected nerves. Muscle weakness is another potential sign. Certain movements, such as coughing, sneezing, or moving into specific positions, may intensify the pain.
How Is One Treated?
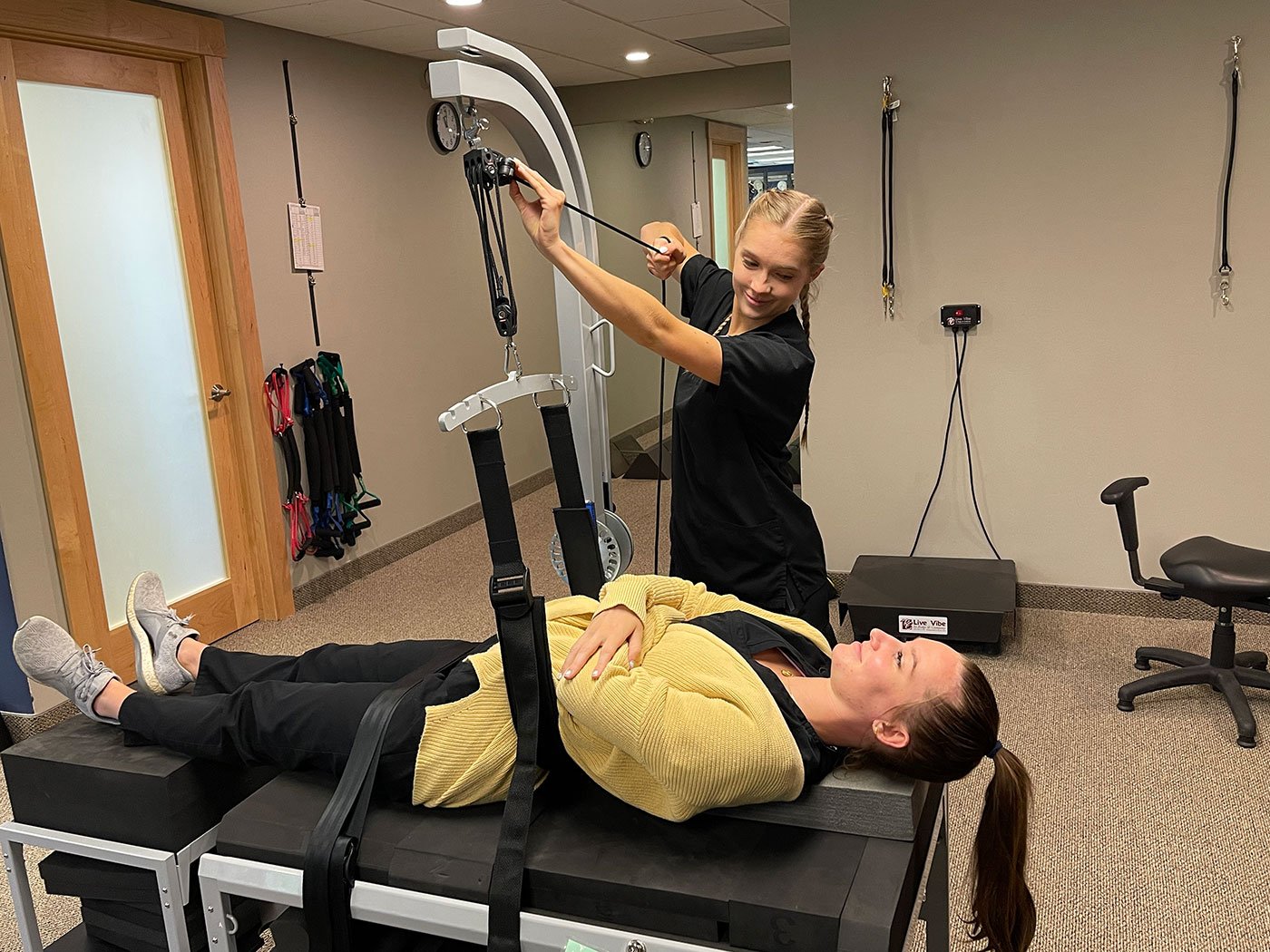
Conservative treatments often start with modifying activities to avoid movements that worsen the pain. Physical therapy can play a role in recovery. Therapists design exercise programs to strengthen the muscles that support the back and improve flexibility. Application of heat or cold packs may also help reduce inflammation.
Pain relievers are frequently used to manage mild to moderate discomfort. Physicians prescribe stronger medications or muscle relaxants in some cases. Corticosteroid injections into the area around the spinal nerves may provide temporary relief by reducing inflammation.
Surgery becomes an option when conservative treatments fail to improve symptoms after several weeks or if the nerve compression causes significant weakness. Surgical procedures aim to remove the protruding portion of the disc or stabilize the spine to relieve pressure on the nerves.
Consult a Spine Specialist
While home remedies and rest can alleviate mild symptoms, persistent or severe pain warrants professional attention. A spine specialist can offer a precise diagnosis through physical examinations and imaging tests. These diagnostic tools allow doctors to pinpoint the exact location and severity of the herniation. Early intervention often leads to better outcomes and prevents the condition from worsening. Specialists can tailor treatment plans to individual needs, helping patients return to their normal activities safely.
- Thriving, Not Just Surviving: Living Well with a Chronic Condition
- Café Culture as a Reflection of Lifestyle Values
- Achieving Facial Symmetry with Botox: A Comprehensive Guide
- How to Choose Safe and Effective Health Supplements
- Smile Confidently Wherever You Travel: How Cosmetic Dentistry Prepares You for Life’s Best Moments