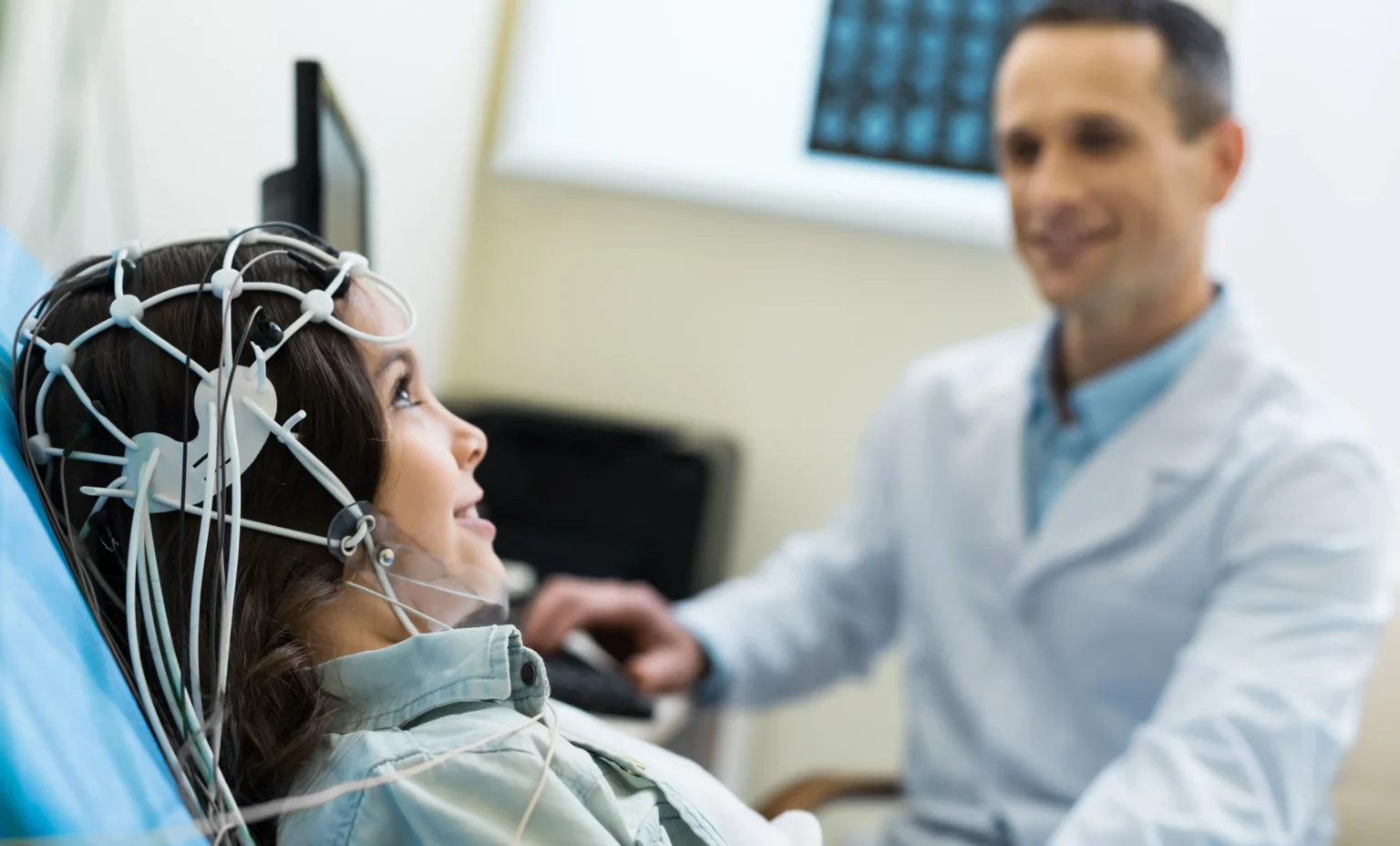
Head Trauma affects patients and their families in complex ways. The effects extend into mental health, daily function, and family life. While the physical aspects may heal, the psychological impact often persists and influences overall recovery. Understanding these challenges requires looking at both the patient’s and the family’s experiences, as both parties can display notable changes in mood, function, and relationships.
Effects of Head Trauma
Individuals who sustain head trauma encounter a range of psychological issues. A concussion causes symptoms such as headaches, dizziness, fatigue, and difficulty focusing. Patients frequently report depression, and studies indicate that depressive symptoms after injury can range from mild to severe. Anxiety is also common, and it occurs due to uncertainty about recovery, concern for future abilities, and worries about returning to work or daily activities; research points to lower scores in these domains compared to non-injured individuals. Although each person’s experience varies, most will observe a change in their emotional state, and these effects can complicate treatments because psychological issues impact motivation and engagement in rehabilitation.
Effects on Family
After head trauma, family and friends are also affected. Family members, especially spouses or partners, often take on caregiving roles, influence daily routines, and provide emotional support. These duties cause stress, and studies find that caregivers report higher rates of depression and anxiety than the general population. Many family members experience emotional distress due to shifts in family dynamics or because their loved one’s personality or behavior has changed. High levels of family communication and a flexible approach can support both the patient and the family, but emotional strain in caregivers remains a common finding and may persist even when other relationships remain stable.
Effects of Treatment
Recovery from traumatic brain injury often requires coordinated, evidence-based care. This care addresses both physical effects and psychological challenges. Outpatient rehabilitation programs typically involve multidisciplinary teams, and these teams may include physicians, therapists, and mental health professionals. Psychological screening for conditions such as depression and anxiety is an essential part of treatment. Counseling may also be recommended, especially when emotional adjustment becomes difficult. Family involvement is emphasized because changes in roles, communication, and daily responsibilities affect both patients and caregivers. Structured, family-centered support can improve overall functioning and reduce caregiver strain.
Support services for caregivers are important for long-term recovery. Education programs provide guidance, and counseling offers emotional support. Support groups help families manage stress and practical challenges related to injury. When depression persists and does not respond to standard treatment, advanced options such as transcranial magnetic stimulation (TMS) may be considered. Early multidisciplinary care, combined with continued access to patient- and family-focused services, supports better mental health outcomes and improves quality of life after head trauma.
Finding Help
Brain injury affects the mental health and daily functioning of both patients and their families, and its psychological impact can be long-lasting. Interventions that address the needs of the whole family, including screening, counseling, and targeted support programs, are necessary in comprehensive care. Understanding and managing these psychological effects helps with outcomes and improved quality of life for everyone involved.
- Thriving, Not Just Surviving: Living Well with a Chronic Condition
- Café Culture as a Reflection of Lifestyle Values
- Achieving Facial Symmetry with Botox: A Comprehensive Guide
- How to Choose Safe and Effective Health Supplements
- Smile Confidently Wherever You Travel: How Cosmetic Dentistry Prepares You for Life’s Best Moments